Infant mortality rates serve as a critical indicator of a nation’s health and well-being, reflecting the disparities that exist within healthcare systems. Alarmingly, recent studies reveal that while life expectancy improves for many, Black and white infant mortality rates have diverged significantly, with Black infants facing twice the risk of mortality compared to their white counterparts. This stark reality underscores the racial disparities in healthcare that persist, highlighting the deep-rooted issues of healthcare inequality in the United States. As researchers demonstrate, the healthcare landscape has evolved, yet these improvements have not extended equitably to all races, particularly in health outcomes for infants. Addressing these disparities is not just a moral obligation but also a necessary step towards improving life expectancy for all racial groups.
The topic of infant mortality rates can also be understood through the lens of neonatal fatality statistics, which reveal harsh realities about the vulnerability of newborns in various demographics. Recent analyses indicate that the gap in mortality figures between Black and white newborns has widened alarmingly, prompting discussions about the systemic issues underlying this phenomenon. Significant concerns related to racial healthcare discrepancies often emerge, illustrating how inequality within medical systems can detrimentally affect the most delicate members of society. As findings show, Black infants are at a disproportionately high risk of dying before their first birthday, a stark contrast to their white peers, raising urgent questions about how to rectify these concerning health outcomes. To create equitable health conditions for all infants, a critical reassessment of policies and resource allocation is essential.
The Alarming Disparity in Infant Mortality Rates
Infant mortality rates represent a critical indicator of a nation’s overall health and wellbeing. Unfortunately, despite advances in healthcare and a general increase in life expectancy, the disparity in infant mortality rates between Black and white Americans has not only persisted but has worsened. Evidence shows that Black infants are dying at double the rate of their white counterparts, an alarming statistic that calls for urgent action. This discrepancy is particularly concerning given the historical context; while overall mortality rates have seen improvements across both racial groups over the past 70 years, the gap in infant mortality reveals deep-rooted systemic issues within the healthcare system.
Moreover, the widening chasm in infant mortality rates highlights broader healthcare inequalities. Medical conditions during pregnancy, access to quality prenatal care, and the social determinants of health all play crucial roles in shaping health outcomes for infants. Despite overall advancements in medical technology and treatments, Black mothers continue to face significant barriers related to healthcare access and quality. Addressing these disparities is imperative if we are to improve the health outcomes for infants and work towards an equitable healthcare system.
Understanding Racial Disparities in Healthcare
Racial disparities in healthcare raise important ethical concerns, especially as they relate to the survival and quality of life of infants. The data shows that while life expectancy for both Black and white Americans has improved, Black infants are disproportionately affected by high mortality rates. This situation emphasizes the roles that systemic racism and healthcare inequality play in shaping outcomes. Numerous factors contribute to these disparities, including socioeconomic status, which heavily influences access to healthcare resources and quality of care.
Further complicating the situation is the fact that many Black families may experience barriers such as inadequate health insurance, limited provider options, and a lack of culturally competent care. All these elements collectively reinforce a cycle of disadvantage that leads to poorer health outcomes for Black infants. Therefore, strategies aimed at reducing these disparities must encompass comprehensive policy changes that focus on providing equal access to high-quality healthcare for all, particularly vulnerable populations.
The Impact of Socioeconomic Factors on Health Outcomes for Infants
Socioeconomic factors play a pivotal role in determining health outcomes for infants. Families with higher socioeconomic status typically have better access to healthcare services, nutritious food, and resources that contribute to healthier pregnancies and infancy. Conversely, families facing economic hardships may struggle with housing instability, food insecurity, and inadequate healthcare access, all of which can exacerbate the risks associated with infant mortality. This relationship between socioeconomic status and health illustrates the need for targeted interventions that address these critical social determinants.
In recognizing the link between socioeconomic factors and health outcomes, policymakers must prioritize investment in community health initiatives that cater specifically to disadvantaged populations. Programs aimed at improving access to prenatal care, nutritional support, and mental health services could significantly reduce the infant mortality rates among Black Americans. By focusing on holistic solutions that address the underlying issues impacting low-income families, we can help ensure healthier starts for infants across racial and economic spectrums.
Addressing Healthcare Inequality for a Better Future
The widening gap in infant mortality rates between Black and white Americans serves as a dire reminder of the persistent inequalities within the healthcare system. While strides have been made in improving overall healthcare outcomes, targeted efforts to reduce healthcare disparities are urgently needed. Policy frameworks must incorporate equity-focused strategies that prioritize vulnerable populations, particularly infants who are at risk of poor health outcomes. By addressing the systemic barriers that hinder access to quality healthcare, we can begin to close the gap and improve health outcomes for Black infants.
In addition, public health campaigns should aim to raise awareness about the importance of equitable healthcare access and advocate for reforms that empower families facing socio-economic challenges. Community-driven approaches that involve stakeholders from affected communities can facilitate better outcomes by ensuring that solutions are tailored to local needs. Ultimately, by comprehensively addressing healthcare inequality, we not only improve the health outcomes for infants but also foster a more equitable society.
The Role of Public Policy in Reducing Infant Mortality
Public policy plays a crucial role in shaping health outcomes, particularly in addressing the disparities evident in infant mortality rates among racial groups. Policymakers must recognize the significance of targeted initiatives aimed at reducing barriers to care and improving access to resources for marginalized populations. It is not enough to merely acknowledge the disparities; actionable steps must be implemented to rectify the systemic inequities that contribute to the higher infant mortality rates faced by Black families.
One effective approach could be the development of policies that promote universal access to healthcare services, including prenatal and postnatal care. Such measures are essential in ensuring that all infants, regardless of race, have the opportunity for a healthy start to life. Additionally, policies need to be designed to support education and preventative care initiatives that empower families with knowledge about healthy practices during pregnancy. By placing a stronger emphasis on equitable public health policies, we can work toward eliminating the unacceptable disparities in infant mortality rates.
The Importance of Comprehensive Data Analysis
Comprehensive data analysis over extensive periods is critical in understanding the trends and patterns related to healthcare disparities, particularly in the context of infant mortality. Researchers have documented the changes in mortality rates among Black and white Americans over 70 years, providing a clear picture of how disparities have evolved. Such longitudinal studies reveal that, while overall mortality rates have improved, the gaps in infant mortality have unfortunately widened, underscoring the importance of continuous data collection and analysis.
Moreover, data analysis not only highlights where disparities exist but also serves as a catalyst for policy reform. Stakeholders can use this information to advocate for evidence-based interventions that target specific populations adversely affected by health inequalities. By aligning research with policy priorities, we can ensure that future initiatives are informed by actual health trends, thus maximizing their potential impact on improving health outcomes for infants.
Cultural Competence in Healthcare Delivery
Cultural competence within healthcare delivery systems is critical in addressing the significant disparities in infant mortality rates among different racial groups. Healthcare providers must be trained to understand and appreciate the cultural backgrounds of their patients, which can influence their access to care and responsiveness to healthcare advice. Knowledge of cultural attitudes and beliefs can improve communication and foster trust between healthcare providers and patients, leading to better health outcomes for infants.
For instance, training programs that focus on cultural awareness can help healthcare providers recognize the unique challenges faced by Black families and develop tailored care plans that address these issues. In turn, improving cultural competence can result in higher rates of healthcare utilization by families who may otherwise feel alienated from the medical system. Addressing the cultural dimensions of healthcare delivery is, therefore, essential for narrowing the healthcare gap and enhancing the overall health outcomes for infants.
Urgent Need for Collaborative Efforts
The issue of infant mortality and the associated racial disparities demand an urgent and collective response from healthcare systems, policymakers, and communities. Collaborative efforts that involve multiple stakeholders, including public health organizations, community advocates, and healthcare providers, are essential to create effective solutions that can close the gap in infant mortality rates. Engaging with affected communities can provide valuable insights into their unique healthcare challenges, leading to the development of tailored interventions.
Furthermore, collaboration is necessary to ensure that health policies address the social determinants of health that disproportionately affect Black families. By pooling resources and knowledge, stakeholders can implement comprehensive initiatives designed to improve access to quality care, nutritional support, and maternal health programs. Only through united efforts can we hope to achieve equitable health outcomes for all infants and ultimately reduce the unacceptable disparities in infant mortality.
Future Directions in Reducing Healthcare Disparities
Looking forward, addressing healthcare disparities in infant mortality means re-evaluating our current approaches and embracing innovative solutions that target the systemic issues at play. Future efforts must focus on both immediate interventions to save lives and long-term strategies that eradicate the root causes of health inequalities. Evidence-based policymaking should be prioritized, utilizing data and research to inform decisions that will lead to meaningful changes in healthcare access and quality.
Additionally, fostering partnerships between public health authorities and community organizations can create sustainable models of care that address the needs of vulnerable populations. Ensuring that policies prioritize health equity will lead to improved health outcomes across racial and socioeconomic lines. The fight against infant mortality must be rigorous, sustained, and inclusive, aimed at building an equitable healthcare landscape where every infant, regardless of race, has an equal chance at a healthy life.
Frequently Asked Questions
What factors contribute to racial disparities in infant mortality rates in the U.S.?
Racial disparities in infant mortality rates in the U.S. are significantly influenced by healthcare inequality, which encompasses issues such as access to quality care, socio-economic factors, and systemic racism. Black infants are currently dying at rates twice that of white infants, with leading causes of excess deaths largely being medical conditions during pregnancy.
How do the infant mortality rates between Black and white infants compare today?
Currently, Black infants have a mortality rate that is 115 percent higher than that of white infants. This disparity has worsened over the decades despite overall improvements in life expectancy for both racial groups.
What roles do public health officials play in addressing healthcare inequality and infant mortality rates?
Public health officials are crucial in addressing healthcare inequality and improving health outcomes for infants. They must prioritize closing the gap in infant mortality rates, particularly between Black and white infants, by implementing policies that ensure equitable access to quality healthcare for all racial groups.
Why is understanding the causes of healthcare inequality important for improving infant mortality rates?
Understanding the causes of healthcare inequality is essential for addressing the widening gap in infant mortality rates. By identifying the specific factors contributing to these disparities, policymakers can develop targeted interventions to improve life expectancy and health outcomes for infants, especially in marginalized communities.
What has recent research shown about the overall trends in life expectancy and infant mortality rates?
Recent research indicates that while life expectancy for both Black and white Americans has improved, the infant mortality rates illustrate a troubling trend where the gap between Black and white infants has widened. Specifically, Black infants are at greater risk, suggesting a need for focused efforts to understand and reduce these disparities.
What can be done to improve health outcomes for infants facing disparities in mortality rates?
Improving health outcomes for infants facing disparities in mortality rates requires comprehensive public health strategies that focus on addressing social determinants of health, enhancing access to quality healthcare, and ensuring equitable resources for all populations, thereby reducing healthcare inequality.
How has public perception of healthcare improvements impacted the approach to infant mortality rates?
Public perception that healthcare improvements have benefitted all populations can overshadow the persistent disparities in infant mortality rates. Acknowledging these gaps is vital for advocating for policy changes and allocating resources effectively to support at-risk groups, particularly Black infants who experience higher mortality rates.
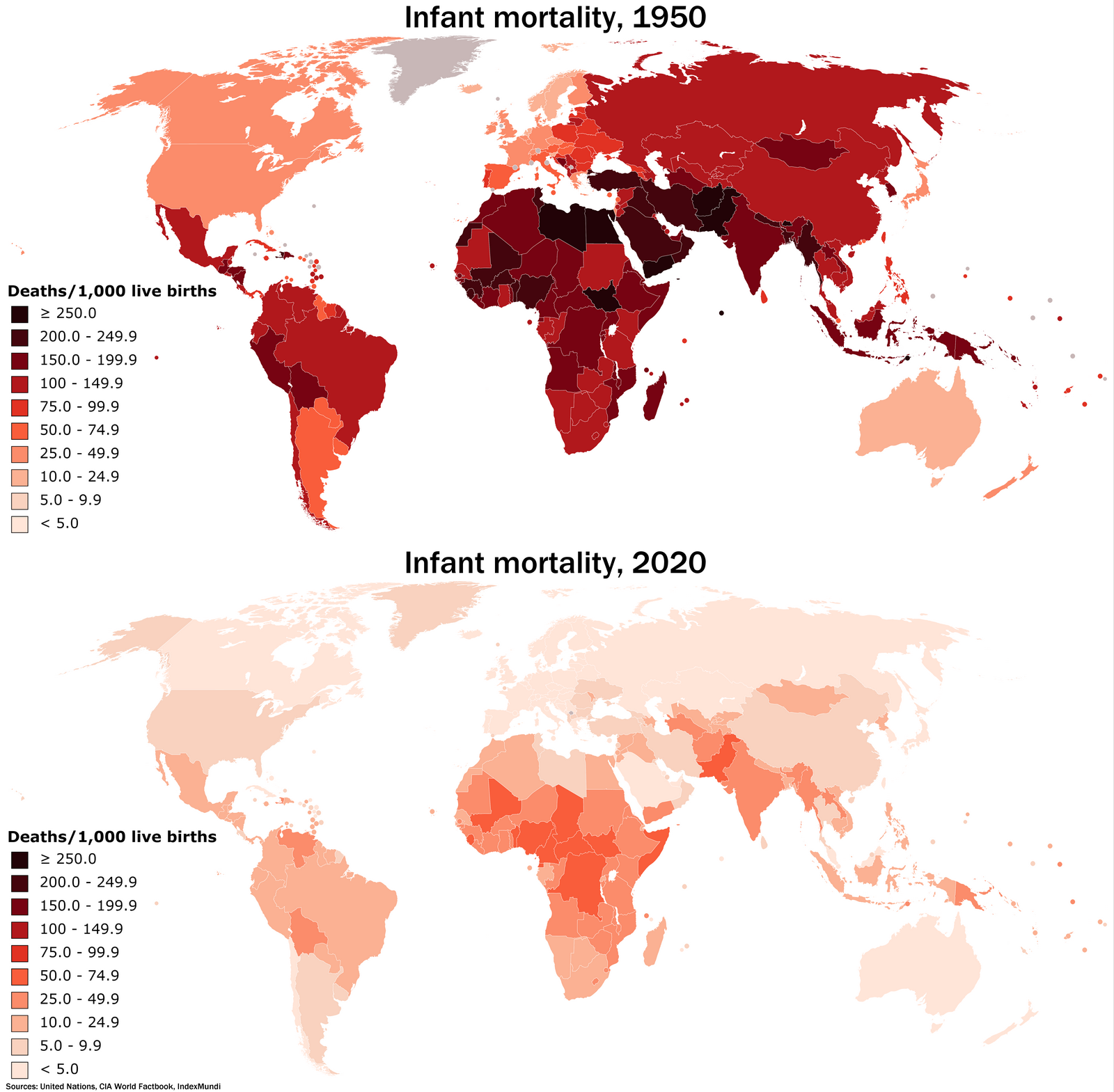
What insights can policymakers gain from studying the trends in infant mortality rates from 1950 to today?
Policymakers can learn that despite improvements in overall health metrics, persistent disparities, particularly in infant mortality rates, demand immediate attention. By analyzing trends from 1950 to today, strategies can be developed to specifically address the needs of Black infants and work towards equitable health outcomes.
| Key Points |
|---|
| Americans’ life expectancy has improved over time, yet significant racial disparities remain in infant mortality rates. |
| Black and white Americans have seen a narrowing gap in overall mortality rates since the 1950s, but the gap for infants has widened. |
| Black infants die at twice the rate of white infants, demonstrating a critical racial disparity in healthcare outcomes. |
| The mortality rate for Black infants was 92% higher than that of white infants in the 1950s, which worsened to 115% today. |
| Medical conditions during pregnancy are the leading causes of excess deaths among Black infants in the 2010s. |
| A comprehensive 70-year study has highlighted persistent inequalities requiring urgent attention from public health policymakers. |
Summary
Infant mortality rates remain a critical public health issue in the United States, with Black infants experiencing significantly higher mortality rates compared to their white counterparts. Despite improvements in overall life expectancy, the widening gap in infant mortality rates highlights ongoing healthcare disparities that demand immediate action. As this study reveals, both public policy and healthcare access must be prioritized to ensure equitable health outcomes for all infants, ultimately striving towards a future where no child is left behind due to the color of their skin.